Thyroid Gland
What is the thyroid gland?
 The thyroid gland is shield-like organ located just below the larynx or Adam's apple. It is a small gland that wraps around the trachea or windpipe. The gland converts iodine from the diet into the thyroid hormone, thyroxine. The levels of this hormone control most of your body's metabolic functions including temperature, heart rate and growth.
The thyroid gland is shield-like organ located just below the larynx or Adam's apple. It is a small gland that wraps around the trachea or windpipe. The gland converts iodine from the diet into the thyroid hormone, thyroxine. The levels of this hormone control most of your body's metabolic functions including temperature, heart rate and growth.
What are the indications for thyroid surgery?
Thyroid surgery (thyroidectomy) may be required if there is:
- A lump that could be a malignant tumour (thyroid cancer). This is usually determined by a fine needle biopsy of the lump.
- A goitre (enlargement of the thyroid) causing pressure on surrounding organs resulting in symptoms such as difficulty swallowing, difficulty breathing or a persistent cough.
- Growth of your thyroid down into the chest cavity (a retrosternal goitre)
- Excessive activity of the thyroid (hyperthyroidism or thyrotoxicosis)
What types of operations are done on the thyroid?
There are various type of thyroid operations that can be done including:
- Total thyroidectomy - removal of the whole thyroid
- Bilateral subtotal thyroidectomy - removal of most of the thyroid leaving part of both lobes behind
- Hemithyroidectomy - removal of half the thyroid
- Excision of thyroid nodule - removal of a lump from the thyroid
If a total thyroidectomy is performed, you will need to take thyroxine tablets for the rest of your life. If less than a total thyroidectomy is performed, you will generally not need to take thyroxine although around 15% of people still require some thyroxine supplementation after just a hemithyroidectomy.
How is thyroid surgery usually done?
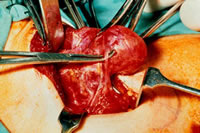 Thyroid surgery is generally performed under a general anaesthetic although it can be done under local anaesthesia in special circumstances if required. An incision is made in the front of the neck, 2 to 3 cm above the collarbone. The underlying muscles are opened or divided to expose the thyroid gland which the surgeon then removes either totally or in part. Great care is taken not to injure the nerves which control the voice box (laryngeal nerves) and every attempt is made to preserve the parathyroid glands which control the body's calcium levels. Sometimes the parathyroid glands may be autotransplanted into a nearby muscle to preserve their function. The muscles are then put together again and the skin incision is closed with sutures that will either absorb or be removed soon after your operation.
Thyroid surgery is generally performed under a general anaesthetic although it can be done under local anaesthesia in special circumstances if required. An incision is made in the front of the neck, 2 to 3 cm above the collarbone. The underlying muscles are opened or divided to expose the thyroid gland which the surgeon then removes either totally or in part. Great care is taken not to injure the nerves which control the voice box (laryngeal nerves) and every attempt is made to preserve the parathyroid glands which control the body's calcium levels. Sometimes the parathyroid glands may be autotransplanted into a nearby muscle to preserve their function. The muscles are then put together again and the skin incision is closed with sutures that will either absorb or be removed soon after your operation.
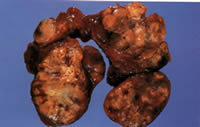 Minimally invasive thyroid surgery (either through a keyhole incision or using an endoscope) is still experimental and should only be performed as part of a recognised trial.
Minimally invasive thyroid surgery (either through a keyhole incision or using an endoscope) is still experimental and should only be performed as part of a recognised trial.
What are the risks and complications of thyroid surgery?
Most surgery nowadays is safe however any operation has general risks including reactions to the anaesthetic, chest infections, blood clots, heart and circulation problems, and wound infection. In addition there are specific risks associated with thyroid surgery as follows:
- Post-operative bleeding may cause swelling in the throat and difficulty breathing due to pressure on the windpipe. It is usually fixed by a further operation to remove the blood clot „h Injury to the laryngeal nerves may cause hoarseness of the voice. This is usually temporary, but may be permanent in up to 1 to 2% of cases. It may improve with speech therapy or further surgery to the vocal cords. If you are a singer or public speaker, any surgery to the thyroid may cause subtle long-term changes to your performing voice.
- If a total thyroidectomy is performed, injury to the parathyroid glands may cause the calcium level in the blood to drop. It is treated with calcium and vitamin D tablets and usually comes good in a few weeks, although up to 1 to 2% of cases will need lifelong calcium supplements.
- A keloid, or overgrowth of scar tissue, may form in any surgical scar. It will result in a tender, pink raised scar but may able to be treated with silicone gel tape or steroid injections.













