Parathyroid Glands
What are the parathyroid glands?
 There are normally four parathyroid glands located near or attached to the back surface of the thyroid just below the larynx or Adam's apple. Each gland is no larger than a grain of rice. These glands secrete parathyroid hormone (PTH) which controls the calcium level in your body.
There are normally four parathyroid glands located near or attached to the back surface of the thyroid just below the larynx or Adam's apple. Each gland is no larger than a grain of rice. These glands secrete parathyroid hormone (PTH) which controls the calcium level in your body.
What are the indications for parathyroid surgery?
Parathyroid surgery (parathyroidectomy) is generally required if there is overactivity of the parathyroid glands, This is either due to a benign tumour of one or more of the glands (parathyroid adenoma), generalised overactivity and growth of all of the glands (parathyroid hyperplasia), or rarely a malignant tumour of one of the glands (parathyroid cancer). Parathyroid overactivity may be associated with loss of calcium from the bones (osteoporosis), generalised tiredness and lethargy, kidney stones, stomach ulcers, aches and pains in the joints, and constipation.
How is parathyroid surgery usually done?
Parathyroid surgery can be done as an open procedure or as a minimally invasive (keyhole) procedure.
Open parathyroidectomy
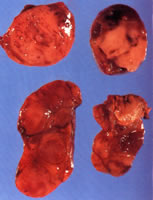 Open parathyroidectomy is generally performed under a general anaesthetic although it can be done under local anaesthesia in special circumstances if required. An incision is made in the front of the neck, 2 to 3 cm above the collarbone. The underlying muscles are opened or divided to expose the thyroid and the parathyroid glands. The surgeon then removes the parathyroid gland or glands that are enlarged. Great care is taken not to injure the nerves which control the voice box (laryngeal nerves). The muscles are then put together again and the skin incision is closed with sutures that will either absorb or be removed soon after your operation.
Open parathyroidectomy is generally performed under a general anaesthetic although it can be done under local anaesthesia in special circumstances if required. An incision is made in the front of the neck, 2 to 3 cm above the collarbone. The underlying muscles are opened or divided to expose the thyroid and the parathyroid glands. The surgeon then removes the parathyroid gland or glands that are enlarged. Great care is taken not to injure the nerves which control the voice box (laryngeal nerves). The muscles are then put together again and the skin incision is closed with sutures that will either absorb or be removed soon after your operation.
Minimally invasive parathyroidectomy
Minimally invasive parathyroid thyroid surgery is performed through a small (2 to 3 cm) keyhole incision directly over the tumour and can be performed under a general or local anaesthetic. It is only suitable for patients where pre-operative scans and tests have been able to identify the exact location of a single parathyroid tumour. Through the small incision the surgeon removes only the enlarged parathyroid, taking great care not to injure the nearby nerves. The skin incision is closed and many patients can go home the same day. In up to 5% of cases, a minimally invasive parathyroidectomy may have to be converted to an open parathyroidectomy if the surgeon cannot locate an enlarged parathyroid gland.
What are the risks and complications of parathyroid surgery?
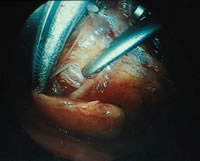 Most surgery nowadays is safe however any operation has general risks including reactions to the anaesthetic, chest infections, blood clots, heart and circulation problems, and wound infection. In addition there are specific risks associated with parathyroid surgery as follows:
Most surgery nowadays is safe however any operation has general risks including reactions to the anaesthetic, chest infections, blood clots, heart and circulation problems, and wound infection. In addition there are specific risks associated with parathyroid surgery as follows:
- Post-operative bleeding may cause swelling in the throat and difficulty breathing due to pressure on the windpipe. It is usually fixed by a further operation to remove the blood clot
- Injury to the laryngeal nerves may cause hoarseness of the voice. This is usually temporary, but may be permanent in up to 1 to 2% of cases. It may improve with speech therapy or further surgery to the vocal cords. If you are a singer or public speaker, any surgery to the thyroid may cause subtle long-term changes to your performing voice.
- Injury to the other parathyroid glands may cause the calcium level in the blood to drop. It is treated with calcium and vitamin D tablets and usually comes good in a few weeks.
- A keloid, or overgrowth of scar tissue, may form in any surgical scar. It will result in a tender, pink raised scar but may able to be treated with silicone gel tapes or steroid injections
- Even in the most expert hands, up to 5% of parathyroid tumours cannot be found at operation and the calcium will remain raised (persistent hyperparathyroidism). Sometimes after successful surgery, one of the other parathyroid glands may also then become overactive and cause the calcium to be raised again (recurrent hyperparathyroidism)













